Diabetic Eye Disease Surgery
What is Diabetic Retinopathy Treatment?
Diabetic retinopathy is a potentially blinding disease.
The retina is the light-sensitive tissue at the back of the eye. A healthy retina is necessary for good vision. Light is focused through the eye onto the retina, allowing us to see. The centre part of the retina is called the macula – it is here that light must be focused for us to see fine detail, to be able to read and to see in colour.
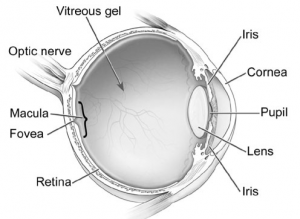
If you have diabetic retinopathy, at first you may not notice changes to your vision. Diabetes causes changes in the blood vessels of the retina and small haemorrhages develop in the retina and macula.
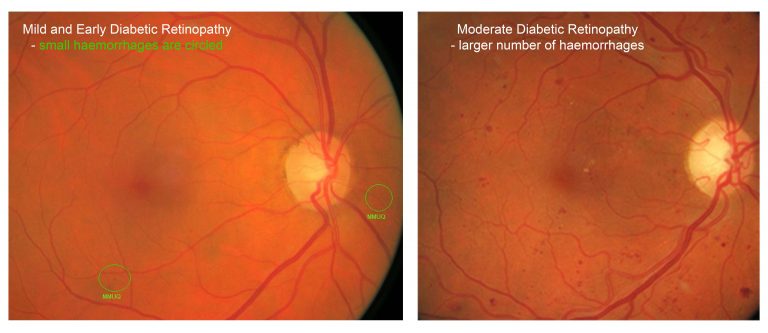
Over time, diabetic retinopathy can get worse and cause vision loss.Diabetic retinopathy usually affects both eyes.
The growth of new vessels leads to bleeding inside the eye and possible retinal detachment with profound global sight loss.
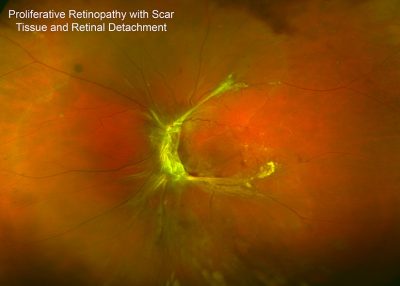
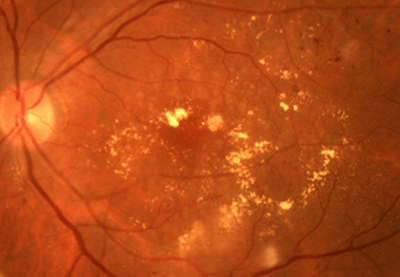
What is the Natural History of Diabetic Eye Disease?
An animation below shows the progression, features, and natural history of diabetic retinopathy.
Your retina specialist and surgeon Mr Mahi Muqit will discuss the natural history of diabetic retinopathy with you, and and explain the warning signs that your eye disease may be progressing and worsening. This individualised approach will help you to understand the impact of your diabetic eye disease on your vision.
Why do I need laser treatment?
Proliferative Diabetic Retinopathy
If you are diabetic and have developed “Proliferative Diabetic Retinopathy”, then harmful new blood vessels have grown on the surface of the retina, the lining at the back of the eye. If left untreated, these abnormal blood vessels can bleed into your eye, cause scarring on the retina, or cause a retinal detachment that can all damage your vision.
A form of laser treatment to the retina has been used to prevent blindness, by causing these new blood vessels to shrink away. The treatment itself involves putting in eye drops which enlarge the pupils (this takes around 20 minutes), and topical anaesthetic eye drops are usually all that is required to keep your eye comfortable during the treatment. Currently, the standard treatment for proliferative diabetic eye disease is laser therapy that is directed to all parts of the retina, but sparing the central area of the retina called the macula. Standard laser treatment is called pan retinal photocoagulation, and Mr Muqit also offers “Targeted Retinal Photocoagulation” therapy for his patients.
The laser light is focused by treating through a contact lens placed on the patient’s eye. You will receive around 5-10 minutes’ worth of treatment in the eye clinic as part of a single session laser therapy. Most patients tolerate the procedure extremely well with little discomfort afterwards.
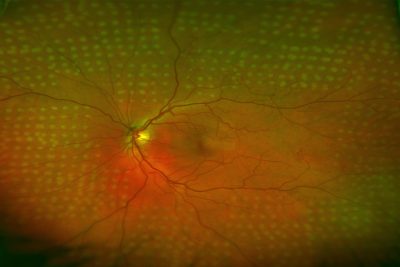
“Mahi Muqit has extensive expertise in laser therapy and has pioneered new laser strategies for diabetic eye disease. You will be treated with innovative and the latest minimally-traumatic laser treatments for your sight-threatening eye disease.”
Why do I need laser treatment?
Diabetic Macular Oedema
If you are diabetic and have developed Diabetic Macular Oedema, then leakage has occurred in the central part of your retina, and the macula has become swollen with fluid. You may be experiencing reduced vision in the form of blurring, darkening or distorted images. Often the amount of macular oedema, and associated symptoms, will be unequal between the two eyes.
In treating diabetic macular oedema, the goal is to help stabilise vision by attempting to stop the damaged blood vessels from leaking fluid into the retina causing it to swell. Usually this form of laser surgery helps stabilise vision rather than improving it (although sometimes it can).
Laser therapy has been demonstrated to allow patients to maintain their vision longer than those left untreated. Both focal and grid laser surgery are used in the treatment of diabetic macular oedema. Focal treatment is possible when there are a small number of discrete areas of leakage which can be targeted directly for treatment. The fluorescein angiogram test is often used as a guide for this procedure. When the leakage is diffuse in nature, laser spots are applied in a grid pattern over the swollen areas of macula.
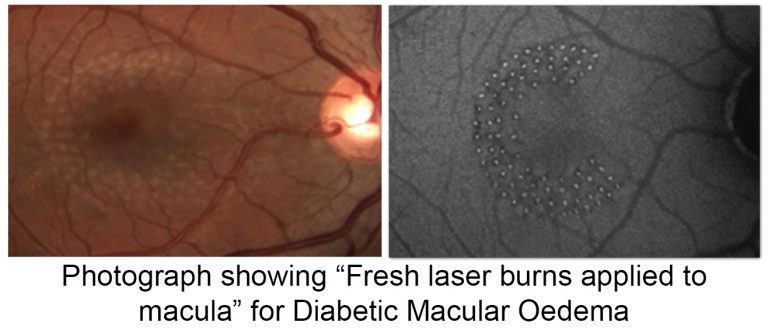
After laser treatment, you may notice small spots in your visual field caused by the laser energy but these spots become less noticeable in a short time. It is important to recognise that the effects of laser are not immediate. It is possible that the vision may get a little worse shortly following laser but, in the long run, most of the patients who receive laser for macular oedema will have better vision than if they had not received the treatment.
What are the Risks of Laser Treatment?
Laser works by the controlled application of laser burns to the macula and retina. The laser spots are applied at the edges of the retina, and blind spots may be found at the edges of the field of vision. Sometimes, if the diabetic eye disease is severe and a lot of laser treatment is needed to both eyes, the visual field is affected, and falls below the legal driving standard. This is unlikely to happen with the new laser treatment strategies. Other risks of laser treatment include light sensitivity, detachment of the retina, leakage of fluid in the back of your eye (macular oedema), and bleeding inside the eye (vitreous and/or pre-retinal haemorrhage). These risks are uncommon.
Surgery for Diabetic Eye Disease
While panretinal photocoagulation is frequently successful in halting the diabetic proliferative process, some patients progress despite laser treatment. Other patients may have bleeding (vitreous haemorrhage) occur before laser can be applied which may prevent laser from being delivered to the back of the eye. The vast majority of vitreous haemorrhages that are due to diabetic retinopathy will be absorbed by the body and clear on their own.
If a vitreous haemorrhage does not clear on its own within six weeks, then early vitrectomy surgery to remove that blood may be indicated. Vitrectomy surgery is also indicated if the abnormal blood vessels and scar tissue contract and pull enough to cause a tractional retinal detachment.
A vitrectomy is a retinal surgery in which the vitreous gel is removed with the aid of micro-incisional surgical instruments in the operating room. Once the vitreous and associated blood is removed, laser is usually added to the side part of the retina during the surgery. Mr Muqit offers “minimally-invasive surgery” for diabetic-related retinal detachments. Small instruments are used to peel the scar tissue off of the surface of the retina to relieve the traction. The goal of surgery is to try to stabilise the vision and decrease the chance of the vision worsening.
Scientific Evidence
The advice in this booklet is based on a variety of sources, including latest research published in peer-reviewed scientific journals and national guidelines. If you require further information, please ask your surgeon. Mr Muqit was an author and part of the expert panel that developed the national Diabetic Retinopathy Clinical Guidelines for The Royal College of Ophthalmologists.
To book an appointment call +44 7717 203564 or email pp@retinasurgeon.uk.com
Treatments & Surgery

Hole
A small, circular gap opens up at the centre of the retina. Causes blurred vision and distorted vision, and patches of missing vision at the centre.

Disease
You must be screened for diabetic retinopathy, as you may not notice changes to your vision. Diabetes damages small blood vessels of the retina, leading to bleeding in the retina and fluid leakage at macula.
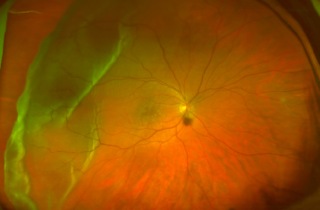
Detachment
The retina is the light sensitive film at the back of the eye and retinal detachment is an emer gency wher e the retina peels away to cause a shadow or loss of vision.

Floaters are shapes that people can see drifting across their vision. Floaters are small bits of debris floating in the vitreous jelly inside the eye.
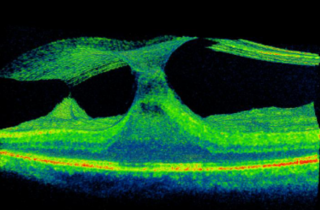
Traction
The vitreous gel shrinks and pulls away from the macula, but the vitreous remains partially stuck and pulls on the macula surface to cause mechanical traction
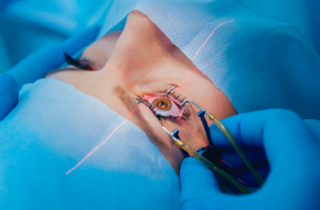
Surgery
Mahi Muqit performs routine and complex cataract surgery for all types of cataract and vitreoretinal patients, and has expertise in lens implant exchange surgery.
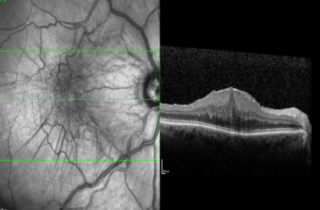
Membrane
Scartissues forms over the Macula, it contracts, crumples, and squashes the Macula resulting in distorted and/or blurred vision.
Surgery
Mahi Muqit performs a wide range of surgical procedures, and offers a comprehensive vitreoretinal surgery service.



